Complications associated with obesity have a significant economic impact on the health care system in the United States, costing $147 billion a year.
Dr. Sung II Park and his collaborators are working on a medical device that could help with weight loss and requires a simpler operative procedure for implantation than current solutions.
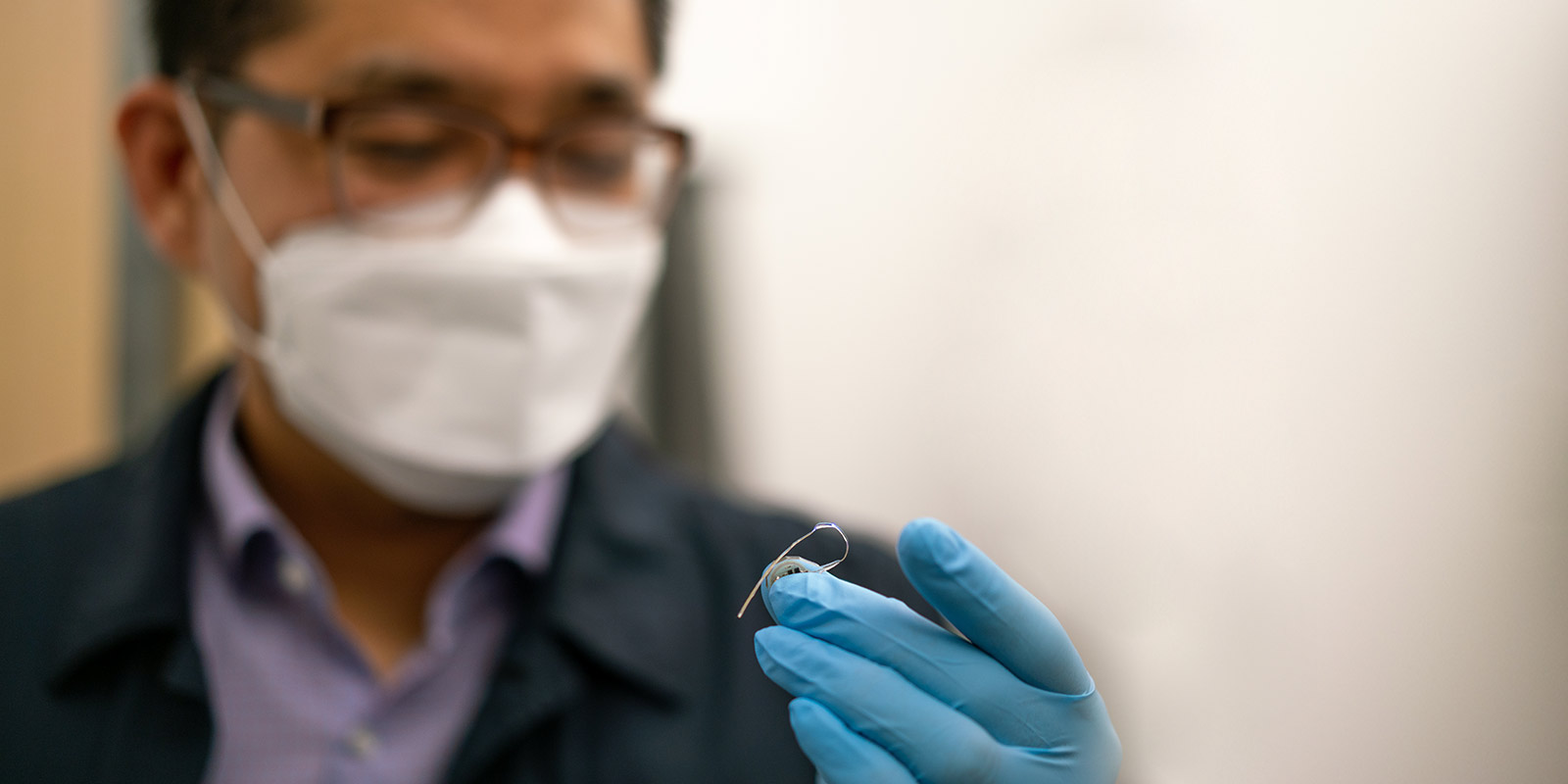
The centimeter-sized device provides the feeling of fullness by stimulating the endings of the vagus nerve with light. Unlike other devices that require a power cord, the team’s device is wireless and can be controlled externally from a remote radio frequency source.
The centimeter-sized device provides the feeling of fullness by stimulating the endings of the vagus nerve with light. Unlike other devices that require a power cord, the team’s device is wireless and can be controlled externally from a remote radio frequency source.
In recent years, the vagus nerve has received much attention as a target for treating obesity since it provides sensory information about fullness from the stomach lining to the brain. Although there are medical devices that can stimulate the vagus nerve endings and consequently help curb hunger, these devices are similar in design to a pacemaker; that is, wires connected to a current source provide electrical jolts to activate the tips of the nerve.
Alternatively, Park said that wireless technology and the application of advanced genetic and optical tools have the potential to make nerve stimulation devices less cumbersome and more comfortable for the patient. He also explained that there is no risk to patients as pacemakers and nerve stimulation devices have been approved by the United States Food and Drug Administration.
“Our novel tool now enables interrogation of neuronal function in the peripheral nervous systems in a way that was impossible with existing approaches,” said Park.
This work has been supported by grants from the interdisciplinary X-Grants Program, a NARSARD Young Investigator Award from the Brain and Behavior Research Foundation, the National Science Foundation’s Engineering Research Center for Precise Advanced Technologies and Health Systems (PATHS-UP), the University of Washington Diabetes Research Center and the National Institutes of Health.
FEATURED RESEARCHER
